Neonatal jaundice is a common condition in newborns, characterized by yellowing of the skin and eyes due to elevated levels of bilirubin in the blood. It is important for parents and healthcare providers to understand the causes, symptoms, diagnosis, and prevention options for neonatal jaundice to ensure the well-being of newborns.
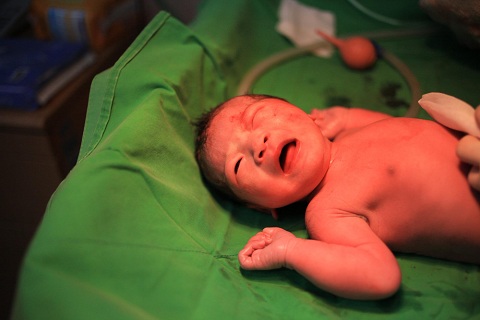
Infantile jaundicerefers to the yellow discoloration of a newborn’s skin and eyes. It occurs due to elevated levels of bilirubin in the blood, a yellow pigment produced by the breakdown of red blood cells. Bilirubin is typically processed by the liver and excreted through bile, but in newborns, this process may be immature, leading to jaundice.
Causes of Infantile Jaundice
- Physiological Jaundice: This is the most common type of jaundice in newborns, occurring as a normal response to the breakdown of fetal red blood cells.
- Breastfeeding Jaundice: Some babies may develop jaundice due to insufficient intake of breast milk, leading to reduced elimination of bilirubin.
- Breast Milk Jaundice: In rare cases, certain substances in breast milk can interfere with bilirubin metabolism, causing prolonged jaundice.
- Blood Group Incompatibility: Isoimmune haemolysis, Rh or ABO blood group incompatibility between the mother and baby can result in increased breakdown of red blood cells and subsequent jaundice.
- Conjugated hyperbilirubinaemia: Hepatic disorders, Neonatal hepatitis as like zellweger’s syndrome it mean anatomic anomaly, metabolic disease, cystic fibrosis, genetic/chromosomal and extrahepatic disorders as like Bile duct stenois, lithiasis, bile or mucous plug, intestianal obsruction, polysplenic syndorme.
- Liver Conditions: Rarely, underlying liver disorders in newborns can contribute to jaundice.
- Other rare cause: It occurs very low casese as like Cretinism, Byler’s disease , Pyloric stenosis, Galactosaemia etc.
Symptoms
Infantile jaundice is characterized by several symptoms, primarily the yellowing of the skin and eyes. This yellow discoloration, known as jaundice, occurs due to elevated levels of bilirubin in the blood. Other common symptoms of infantile jaundice include:
- Yellowing of the skin: The most noticeable symptom, where the baby’s skin appears yellow, especially on the face, chest, abdomen, and legs.
- Yellowing of the eyes: The whites of the eyes (sclera) may also turn yellow, known as scleral icterus.
- Pale stools: Infants with jaundice may have pale or clay-colored stools, which indicate a disruption in the normal bile flow.
- Dark urine: Jaundiced babies often pass urine that is dark in color, ranging from amber to brown, due to the presence of excess bilirubin.
- Poor feeding: Some babies with jaundice may show signs of decreased appetite, feeding difficulties, or increased sleepiness.
- Lethargy: Infants with severe jaundice may appear lethargic, less active, and have reduced muscle tone.
Diagnosis and Testing
- Bilirubin Levels: Blood tests are used to measure bilirubin levels in the baby’s blood.
- Physical Examination: Doctors may perform a physical exam to assess the extent of jaundice.
- Blood Tests: Additional blood tests may be conducted to identify underlying causes.
10 Tips for Dealing with Infantile Jaundice
- Regular Check-ups: Ensure that your baby receives regular check-ups with a healthcare provider to monitor bilirubin levels and assess overall health.
- Breastfeed Frequently: Breastfeeding helps to flush out excess bilirubin from your baby’s system. Feed your baby at least 8 to 12 times a day, or as recommended by your healthcare provider.
- Monitor Urine and Stool: Keep track of your baby’s urine output and stool color. Dark urine and pale stools may indicate elevated bilirubin levels.
- Follow Phototherapy Guidelines: If your baby requires phototherapy, follow the healthcare provider’s instructions regarding the duration and frequency of light exposure.
- Encourage Sunlight Exposure: Gentle exposure to natural sunlight can also help reduce bilirubin levels. Place your baby in indirect sunlight for short periods, avoiding direct sunlight to prevent sunburn.
- Stay Hydrated: Ensure that your baby stays well-hydrated by offering frequent breastfeeding or formula feeds. Adequate hydration supports the elimination of bilirubin through urine.
- Monitor Weight Gain: Keep track of your baby’s weight gain to ensure they are getting enough nutrition. Consult with a healthcare provider if there are concerns about feeding or weight gain.
- Use Biliblankets if Advised: In some cases, healthcare providers may recommend using biliblankets at home to provide continuous phototherapy. Follow the instructions provided by your healthcare team.
- Seek Support: Dealing with infantile jaundice can be stressful. Seek support from family, friends, or support groups to cope with any emotional challenges.
- Follow-up Care: After the jaundice resolves, continue to follow up with healthcare providers for regular check-ups and monitoring to ensure your baby’s ongoing health and development.
When should I seek medical help for infantile jaundice?

You should seek medical help for infantile jaundice if:
- Jaundice persists beyond two weeks: While mild jaundice is common in newborns and often resolves within a week or two, persistent jaundice may indicate an underlying issue that requires medical evaluation.
- Jaundice is severe: If your baby’s skin and eyes appear significantly yellow or if they have other symptoms such as lethargy, poor feeding, or dark urine, it’s important to seek prompt medical attention.
- Jaundice develops within the first 24 hours: Early-onset jaundice (within the first 24 hours after birth) can sometimes be a sign of a more serious condition, such as blood group incompatibility or hemolytic disease, requiring immediate medical assessment.
- You’re concerned about your baby’s health: Trust your instincts as a parent. If you have any concerns about your baby’s health, including jaundice, it’s best to consult with a healthcare provider for guidance and appropriate care.
Risk Factor for infanile jaundice
Infantile jaundice can occur due to various factors, and certain risk factors may increase the likelihood of its development. Here are some common risk factors for infantile jaundice:
- Prematurity: Babies born prematurely, before 37 weeks of gestation, have an increased risk of developing jaundice because their liver may not be fully matured to process bilirubin efficiently.
- Breastfeeding: Breastfeeding jaundice can occur in newborns who are exclusively breastfed. This type of jaundice is usually mild and occurs within the first week of life due to factors like inadequate milk intake or insufficient calorie intake from breast milk.
- Blood Type Incompatibility: ABO or Rh blood group incompatibility between the mother and baby can lead to an increased breakdown of red blood cells in the baby, resulting in higher bilirubin levels and jaundice.
- Previous Sibling with Jaundice: If a previous sibling had jaundice, especially if it required treatment with phototherapy or exchange transfusion, there may be a higher risk for subsequent siblings to develop jaundice.
- East Asian or Mediterranean Descent: Babies of East Asian or Mediterranean descent have a higher prevalence of a genetic condition called G6PD deficiency, which can lead to jaundice due to increased red blood cell breakdown.
- Bruising or Birth Trauma: Babies who experience bruising or birth trauma during delivery may have increased red blood cell breakdown, leading to higher bilirubin levels and jaundice.
- Infection: Certain infections, such as sepsis or urinary tract infections, can contribute to jaundice in newborns by affecting liver function or increasing red blood cell breakdown.
- Certain Medications: Some medications given to the mother during pregnancy or to the baby after birth can affect bilirubin levels and contribute to jaundice.
FAQs About Infantile Jaundice:
Mild cases are usually harmless, but severe jaundice can lead to complications such as brain damage.
Yes, newborns can recover from jaundice. Most cases of infantile jaundice are mild and resolve on their own within a week or two without long-term consequences. However, severe or prolonged jaundice may require medical intervention and monitoring.
While not always preventable, proper prenatal care and monitoring can reduce the risk.
Yes, sunlight can help in the treatment of jaundice, specifically through a process called phototherapy.
Yes, babies with jaundice may sleep more than usual. Jaundice can sometimes cause lethargy or sleepiness in newborns.
Conclusion
While infantile jaundice is common and usually resolves on its own, timely diagnosis and appropriate management are crucial to prevent complications. By understanding the causes, symptoms, diagnosis, and preventive measures outlined in this guide, parents and healthcare providers can work together to ensure the well-being of newborns affected by jaundice.